Presentation LBP UMI
-
Upload
jhost-clinton-purba -
Category
Documents
-
view
236 -
download
0
Transcript of Presentation LBP UMI
-
7/28/2019 Presentation LBP UMI
1/47
DISEASE OF SPINE
LUHU A. TAPIHERU
-
7/28/2019 Presentation LBP UMI
2/47
Topik
LBP HNP, Lumbar spinal stenosis
Spondilitis TB
-
7/28/2019 Presentation LBP UMI
3/47
LBP (Low Back Pain)
Life time prevalence 59%
10% leads to consultation to GP
90% improved in 1 month
up to 70% patient tend to recur
EPIDEMIOLOGY
-
7/28/2019 Presentation LBP UMI
4/47
Non-specific mechanical back pain Facet joint syndrome
Lumbar disc degeneration (lumbar spondylosis)
Lumbar disc prolapse
Spondylolisthesis
Spinal stenosis
Osteoporosis
Sero-negative spondyl arthritis (includingankylosing spondylitis)
Vertebral infection Disc space infection
Malignancy secondary myeloma and primary
Pagets disease, referred-visceral,pancreatic/pelvic, etc
Etiology
-
7/28/2019 Presentation LBP UMI
5/47
RED FLAGS (possible serious spinal pathology)
Age of onset : < 20 or 55 years
Violent trauma, eg fall from a height, traffic
accident
Constant, progressive, non-mechanical pain
Thoracic pain
History of carcinoma Systemic steroids
Drug abuse, HIV infection
Systemically unwell
Weight loss Persistent severe restriction of lumbar flexion
Widespread neurological deficit
Structural deformity
-
7/28/2019 Presentation LBP UMI
6/47
1. Mechanical (deformity, trauma)
2. Inflammation
3. Neoplasm
4. Degenerative
5. Psychological
COMMON ETIOLOGY
-
7/28/2019 Presentation LBP UMI
7/47
Ligamentous Strain
Muscle strain or spasm
Facet join disruption or degeneration
Intervertebral disc degeneration or herniation Vertebral compression fracture
Vertebral end-plate microfractures
Spondylolisthesis
Spinal stenosis Diffuse idiopathic skeletal hyperostosis
MECHANICAL
-
7/28/2019 Presentation LBP UMI
8/47
SPONDYLOSIS, SPONDYLOLISIS AND
SPONDYLOLISTHESIS
SPONDYLOSIS :
refers to osteoarthritis involving the articular
surfaces (joints and discs) of the spine, often with
osteophyte formation and cord or root compression
SPONDYLOLISIS :
refers to a separation at the pars articularis, which
permits the vertebrae to slip. Maybe uni or bilateral
-
7/28/2019 Presentation LBP UMI
9/47
SPONDYLOSIS, SPONDYLOLISIS AND
SPONDYLOLISTHESIS
SPONDYLOLISTHESIS :
May result from bilateral pars defects or
degenerative disc disease.
Defined as the anterior subluxation of thesuprajacent vertebrae, often producing central canal
stenosis : it is the slipping forward of one vertebrae
on the vertebrae below.
-
7/28/2019 Presentation LBP UMI
10/47
Epidural abcess
Vertebral osteomyelitis
Septic discitis
Potts disease (tuberculosis)
Nonspecific manifestation of systemic illness
INFECTION
-
7/28/2019 Presentation LBP UMI
11/47
Epidural or vertebral carcinomatous
metastases Multiple myeloma
Lymphoma
NEOPLASM
-
7/28/2019 Presentation LBP UMI
12/47
-
7/28/2019 Presentation LBP UMI
13/47
HNP
-
7/28/2019 Presentation LBP UMI
14/47
HNP
HNP : Hernia Nukleus Pulposus
Sinonim : Ruptured disk, prolapsed disk, herniadiskus intervetrebralis
Penyebab NPB (Nyeri punggung bawah) / LBP(low back pain) yang penting
Prevalensi 1 2% dari populasi
90%diskus intervetebralis L5 S1 aan L4
L5 Biasanya membaik 6 minggu
-
7/28/2019 Presentation LBP UMI
15/47
HNP
Definisi :
Suatu keadaan dimana sebagian atauseluruh bagian nukleus pulposus mengalami
penonjolan ke dalam kanalis spinalis
HNP :
HNP servikalis HNP lumbalis
HNP torakalis
-
7/28/2019 Presentation LBP UMI
16/47
The disc
-
7/28/2019 Presentation LBP UMI
17/47
Herniated disc
-
7/28/2019 Presentation LBP UMI
18/47
Patofisiologi
Diskus intervetebralis penyangga beban(Shock absorber)
Terdiri dua bagian utama :
1. Anulus fibrosus : lapisan luar fibro-kolagenyang saling menyilang, bagian dalam lapisan
fibro-kartilagenus
2. Nukleus pulposus : terdiri dari proteoglycan
yang terdiri dari 80% air (higroskopis)
-
7/28/2019 Presentation LBP UMI
19/47
HNP Lumbalis
1. L5 S1 tugas berat menyangga berat badan (75%)
2. Mobilitas tinggi pada fleksi dan ekstensi. 57%aktivitas fleksi dan ekstensi dilakukan sendi
L5 - S13. Daerah rawanligamentum longitudinalis
posterior hanya separuh menutupi permukaanposterior diskus arah herniasi postero lateral
-
7/28/2019 Presentation LBP UMI
20/47
Derajat HNP
Protruded disk: penonjolan nukleus pulposus tanpa
kerusakan annulus fibrosus
Prolapsed disk: nukleus berpindah tetapi tetap
dalam lingkaran annulus fibrosus.
Extruded disk: nukleus keluar dari annulus fibrosus
dan berada di bawah ligamentum longitudinalis
posterior.
Sequestrated dis k: nukleus telah menembus
ligamentum longitudinalis posterior.
-
7/28/2019 Presentation LBP UMI
21/47
Grade of herniated disc
-
7/28/2019 Presentation LBP UMI
22/47
Clinical symptoms
Lumbar HNP :
radicular pain
abnormal vertebral posture
paresthesia, parese, diminished tendon reflexes Cervical HNP :
radicular pain, aggravated by neck extension,
and reduced by abducting the arm and put it
behind the head
paresthesia, parese, diminished tendon reflexes
-
7/28/2019 Presentation LBP UMI
23/47
Ischialgia (sciatic)
-
7/28/2019 Presentation LBP UMI
24/47
Diagnosis
Anamnesis
Neurological examination Sensorik, motorik, reflek
Lumbar HNP : Lasegue (SLR = straight leg raising) test
Lasegue + provokasi Bragard
Crossed Laseque (crossed SLR) test
Femoral stretch (reverse SLR) test Cervical HNP :
Lhermitte test
Valsava test
Shoulder abduction test
-
7/28/2019 Presentation LBP UMI
25/47
Diagnosis
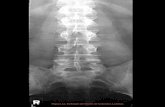
Pemeriksaan radiologis : Plain vertebral x-rays :
limited information
disc narrowing, scoliosis, lordosis lumbal
Myelography
CT or CT-myelography
MRI
EMG/NCV : 90% abnormal after 1-2 weeks
-
7/28/2019 Presentation LBP UMI
26/47
Therapy
CONSERVATIVE bed rest
analgetic, muscle relaxant, ajuvant analgentics
orthopaedic mattress
pelvic traction (controversial)
lumbar corset
OPERATIVE
Indication :1. Fail conservative treatment
2. Progressive motor dysfunction
3. Recurrence
4. Compression of cauda equina
5. Bowel disorders
-
7/28/2019 Presentation LBP UMI
27/47
Sebagian besar membaik dalam 6 minggu
Sebagian kecil kronik Post Op 90% membaik, rekurensi 5%
Prognosis
-
7/28/2019 Presentation LBP UMI
28/47
Spinal stenosis
-
7/28/2019 Presentation LBP UMI
29/47
Lumbar spinal stenosis
CLINICAL SYMPTOMS :
neurogenic intermittent claudiation or
pseudoclaudication (most frequent)
usually bilateral, but maybe unilateral a dull, aching pain
the whole lower extremity is generally affected
pain provoked by walking and standing, quickly
relieved by sitting or leaning forward LBP presents in 65% patients with lumbar spinal
stenosis
radicular pain is the least common manifestation
-
7/28/2019 Presentation LBP UMI
30/47
-
7/28/2019 Presentation LBP UMI
31/47
Most frequent causes of spinal stenosis
> 25 causes are identified
The most common :
1. Idiopathic : the result of shorter than normal
pedicles, thickened convergent lamina, and a
convex posterior vertebral body.
2. Degenerative (50% of cases) : degenerative
changes affect the facets posteriorly allowing
instability and subluxation, osteophytes form
and narrow the nerve root and the central canal; and the disc anteriorly allowing the disc to
bulge into the nerve root and central canal.
-
7/28/2019 Presentation LBP UMI
32/47
most frequent causes of spinal stenosis
3. Degenerative spondylolisthesis : occurs whenthe facets degenerate, allowing slippage of theupper vertebrae forward over the lowervertebrae.
4. Postoperative : occurs after laminectomy orspinal fusion. Stenosis is produced by boneformation and scar tissue
-
7/28/2019 Presentation LBP UMI
33/47
Indication for surgical treatment of
lumbar spinal stenosis
1. Persistent intolerable pain
2. Limitation of walking distance or standing
endurance to a degree that compromises necessary
activities
3. Severe or progressive muscle weakness or
disturbed bladder of sexual function.
-
7/28/2019 Presentation LBP UMI
34/47
Spondilitis TB
-
7/28/2019 Presentation LBP UMI
35/47
Spondilitis TB
Spondilitis TB, s inon im :
Tuberkulosis spinal
Potts disease
Tubercu losis vertebral os teomyel i t is
Mr. Pervical Pott (1779)
Insiden berhubfasilitas pelayanankesehatan dan keadaan sosial
-
7/28/2019 Presentation LBP UMI
36/47
Epidemiologi Spondilitis TB
Di Asia 50% usia 1 20 tahun Keterlibatan tulang sendi pada pasien TB
10% 50 % mengenai vertebra (Vt thorakal 9 - 10),
sisanya tulang panggul, lutut dan tulang kaki
lainnya
Penyebab paling sering paraplegia non
traumatik
-
7/28/2019 Presentation LBP UMI
37/47
Patogenesis spondilitis TB
Penyebaran spondilitis TB Hematogen
Langsung nodus limfatikus para aorta dan jalurlimfatikus
Sumber infeksi sistema pulmoner dangenitourinarius
Penyebaran melalui : arteri interkostal / lumbar suplai darah ke dua
vertebrae yang berdekatan (setengah bagianbawah vertebra diatasnya dan bagian atasvertebra di bawahnya)
-
7/28/2019 Presentation LBP UMI
38/47
pleksus Batsonsmengelilingi columnavertebralismenyebabkan banyak vertebra yangterkena
Tiga bentuk spondilitis TB (lokasi infeksi
pada korpus)
Paradiskal
Sentral
Anterior : adanya scal loped =bentuk baji(erosinya bagian anterior beberapa vertebra)
Atipikal
Patogenesis spondilitis TB
-
7/28/2019 Presentation LBP UMI
39/47
-
7/28/2019 Presentation LBP UMI
40/47
Gambaran klinis spondilitis TB
Potts paraplegia
Early onset : < 2 tahun
Late onset : 2 tahun
Paraplegia : Akibat tekanan eksternal (pd med. Spinalis dan
duramater)
Invasi duramater (tdp gambaran meningomielitis
TB / araknoiditis TB) Disertai inkontinesia urin dan alvi, gangguan
sensoris
-
7/28/2019 Presentation LBP UMI
41/47
Diagnosis spondilitis TB
Anamnesis :
Kehilangan BB, riw. batuk lama, keringat malam
hari, demam intermiten, cachexia
Nyeri : lesi torakal atas
nyeri dada interkostal,lesi torakal bawahnyeri penjalaran ke perut Punggung kaku
Pemeriksaan fisik:
Deformitas : kifosis, gibbus, skoliosis, subluksasi,spondilolisthesis dan dislokasi
Paraparesis UMN, spastisitas,
-
7/28/2019 Presentation LBP UMI
42/47
-
7/28/2019 Presentation LBP UMI
43/47
-
7/28/2019 Presentation LBP UMI
44/47
Lama pemberian ; Menurut Gilroy :
Initial treatment (2 bln) : R, INH, PZA
Continued treatment (9 bln) : R, INH
Menurut Pengobatan TB paru, terbagi 2 fase
1. Fase intensif (2-3 bulan)
2. Fase lanjutan (4-7 bulan)
3. Istirahat tirah baring
Manajemen terapi spondilitis TB
-
7/28/2019 Presentation LBP UMI
45/47
Indikasi operatif Diagnosa yang meragukan hingga diperlukan untuk
melakukan biopsi
Terdapat instabilitas setelah proses penyembuhan
Terdapat abses yang dapat dengan mudahdidrainase
Untuk penyakit yang lanjut dengan kerusakantulang yang nyata danmengancam atau kifosis
berat saat ini Penyakit yang rekuren
Manajemen terapi spondilitis TB
-
7/28/2019 Presentation LBP UMI
46/47
1. Mortalitas menurun sejak ditemukannyakemoterapi TB
2. Relaps 0% (pengawasan ketat pemberian regimen)
3. Kifosis deformitas, masalah kosmetik4. Defisit neurologis membaik (tu. Operasi dini)5. Usia dini prognosis lebih baik6. Fusi tulanghal yang penting untuk pemulihan
Prognosis spondilitis TB
-
7/28/2019 Presentation LBP UMI
47/47